Heat Related Emergencies
HEALTH 103.101
Paul Enkiri
What is a Heat-Related Emergency?
Given the right, or wrong, conditions, anyone can develop heat-illness
Heat-related emergencies occur when the human body is unable to get rid of excess heat fast
There are 3 recognized heat-related illnesses: heat cramps, heat exhaustion, and heat stroke
Heat Cramps
Occurs during or after physical exertion, usually when performing heavy exercise in the heat while sweating profusely and drinking non-electrolyte-containing water
Heat Cramps are defined as painful muscle spasms that happen suddenly; affecting the muscles in the back of the leg or abdomen
Caused by inadequate circulation to the muscles
Treatment for Heat Cramps
3) stretch the cramped calf muscle, and place an ice bag on the painful muscle
1) have the victim rest in a cool place
2) have the victim drink lightly salted, cool water, or sports drink diluted with water so it isn’t as sugary

Heat Exhaustion
Because blood flow is redirected to the skin and muscles, circulation to the brain is impaired, leading to Heatstroke
Heat Exhaustion is characterized by: heavy perspiration with slightly above normal body temperature; the heavy sweating cause water and electrolyte loss, causing severe dehydration
Affects those who do not drink enough fluids while working or exercising in hot environments
Heat Exhaustion (Continued)
Signs and Symptoms
- sweating
- thirst
- fatigue
- flulike symptoms (headache/nausea)
- shortness of breath
- fast heart rate

Treatment for Heat Exhaustion
1) Move victim immediately to cool place
2) Give cool liquids to replace lost electrolytes
3) Consider raising the victims legs 6 - 12 inches (slightly bent)
4) Remove excess clothing
5) Sponge victim with cool water/ fan them/ place ice bags on sides of chest, armpits and neck
6) If no improvement within 30 minutes, seek medical care
Heatstroke
Heatstroke can be defined into two categories:
- Classic heatstroke: slow cooker; can take days to develop; results from a combination of a hot environment and dehydration
-
External heatstroke: fast cooker, more common in the summer; affects those working or playing in warm environments; rapid onset doesn’t allow enough time for dehydration, just heavy sweating.
Heat Stroke
Telling the Difference Between Heat Exhaustion and Heatstroke
- victim’s body is extremely hot to the touch
- altered mental status
- coma in severe cases
- rectal temperature can help distinguish the difference

Treatment for Heatstroke
- 1) Move victim immediately to a cool place
- 2) Remove clothing down to the victim’s underwear
- 3) Keep the victim’s head and shoulders slightly elevated
- 4) Call 9-1-1 immediately even if the victim is recovering
- 5) Cool the victim quickly by any means possible
- Spray the victim with water and then fan (not effective in high humidity)
- Apply cool wet sheets or cloth
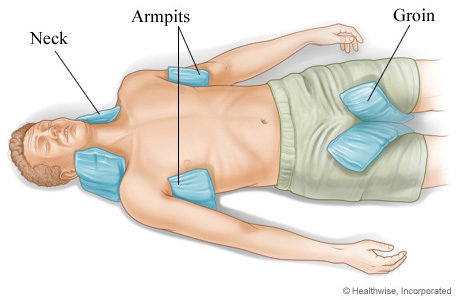
- Place ice bags against large veins on the groin, armpit, and sides of neck
- Place the victim in an ice bath (quick method)
- Place victim in cool water bath
Who is at Risk?
Everyone is susceptible to heat illness if environmental conditions overwhelm the body’s thermoregulation, (temperature regulating mechanism).
Several groups are at risk, including: the obese, those with chronic illness, alcoholics, the elderly, infants, children, and pets.
Who is at Risk? (Continued)
These features reduce children's ability to dissipate body heat by evaporation:
- Children have a greater body surface area-to-mass ratio compared to adults, allowing greater heat transfer between the environment and the body
- Children produce more metabolic heat and have less efficient cooling mechanisms compared to adults
- Children have more sweat glands, but their sweat gland size is smaller
- They sweat less and have a higher threshold for sweating compared to adults
Who is at Risk? (Continued)
Intrinsic Risk Factors:
- poor fitness
- dehydration
- lack of sleep
- illness
- overzealousness
- genetic predisposition
Extrinsic Risk Factors:
- high WBGT (Wet-bulb Global Temp.
- excess clothing/equipment
- lack of acclimation
- lack of medical supervision
How the Body Stays Cool
The human body maintains a steady body temperature of 98.6* Fahrenheit. If your body is unable to get rid of excess heat fast enough, it cooks the brain and other vital organs, often causing fatal injuries, or permeant damage.
Two main ways for the body to get rid of excess heat:
- When the air is 70* F or less, the body releases heat into it’s surroundings through Radiation
- Evaporation occurs when heat is lost through sweating. Water makes up about 50% of the body’s weight.
How the Body Stays Cool (continued)
To stay hydrated while working, especially in hot weather, you should drink 8 ounces of water about every 20 minutes.
You loose about 2 quarts of water every day through breathing, sweating, urinating, and bowel movements.
Electrolyte loss happens through sweat and urine. Electrolytes like potassium and sodium are essential to moving water in and out of the cells. It is important to maintain a balance of electrolytes in order for the body to properly maintain a normal body temperature.
How the Body Stays Cool (continued)
Effects of humidity:
- Sweat cools the body only if it evaporates.
- This can only happen in dry air
- if the humidity is above 75%, seating becomes ineffective in cooling the body
- The higher the humidity, the lower the temperature at which heat risk begins, especially people doing vigorous work
Prevention of Heat-Related Emergencies
1) Primary prevention:
- having predetermined criteria when event activities are curtailed, or cancelled due to environmental conditions that could precipitate heat-related illnesses
- Primary prevention also includes education of children, families, coaches, and emergency responders on the risk factors for heat-related illnesses, their signs and symptoms, and how to recognize and treat affected children

Prevention of Heat-Related Emergencies (continued)
2) Secondary prevention:
- the early detection of, or screening for, heat-related illnesses
- Youth, family, coaches, and emergency personnel should be able to screen spectators and players for signs of heat-related illnesses.
3) Tertiary prevention:
- the rapid diagnosis and treatment of children with heat-related illnesses.
Recent Medical Findings
Cardiovascular Responses to Heat Stress in Chronic Heart Failure
- Clinical reports have suggested that patients with heart diseases may be particularly vulnerable to heat injury
- cardiovascular conditions associated with ventricular dysfunction and chronic heart failure (CHF) are predisposed to heat intolerance
- heat-dissipating responses are accompanied by critical cardiovascular adjustments, which are under autonomic control
- If these adjustments are ineffectual, then thermal regulation can be compromised during exercise and/or exposure to elevated environmental temperatures
- On the other hand, heat exposure, as a stimulus to the cardiovascular system, has been suggested as a therapeutic intervention in patients with cardiovascular diseases including CHF
Recent Medical Findings (Continued)
Cardiovascular Responses to Heat Stress in Chronic Heart Failure
Conclusions:
- Skin and sweating responses to heat stress are impaired in patients with CHF
- It is clear that heat waves increase the risk of cardiac illness
- It is also important to note that modest heat exposure might be beneficial in patients with cardiac disease. Heat therapy will need to be understood better and tested in subjects with CHF.
The End
Citations
Thygerson, Alton L., and Steven M. Thygerson. First Aid, CPR, and AED. 6th ed. Sudbury, Mass.: Jones & Bartlett Learning, 2012. Print.
Pryor, Riana R, et al. "Exertional Heat Stroke: Strategies for Prevention and Treatment From the Sports Field to the Emergency Department." Clinical pediatric emergency medicine 14.4 (2013):267-278.
http://sfx.umd.edu/tusid=Elsevier%3AScopus&_service_type=getFullTxt&issn=15228401&isbn=&volume=14&issue=4&spage=267&epage=278&pages=267278&artnum=&date=2013&id=doi%3A10.1016%2Fj.cpem.2013.10.005&title=Clinical%20Pediatric%20Emergency%20Medicine&atitle=Exertional%20Heat%20Stroke%3A%20Strategies%20for%20Prevention%20and%20Treatment%20From%20the%20Sports%20Field%20to%20the%20Emergency%20Department&aufirst=R.R.&auinit=R.R.&auinit1=R&aulast=Pryor
Citations (continued)
Bernardo, Lisa M, Patricia ACrane, and Tener GVeenema. "Treatment and Prevention of Pediatric Heat-related Illnesses at Mass Gatherings and Special Events." Dimensions of critical care nursing 25.4 (2006):165-171.
http://sfx.umd.edu/tusid=Elsevier%3AScopus&_service_type=getFullTxt&issn=07304625&isbn=&volume=25&issue=4&spage=165&epage=171&pages=165171&artnum=&date=2006&id=doi%3A10.1097%2F0000346520060700000008&title=Dimensions%20of%20critical%20care%20nursing%20%3A%20DCCN&atitle=Treatment%20and%20prevention%20of%20pediatric%20heatrelated%20illnesses%20at%20mass%20gatherings%20and%20special%20events.&aufirst=L.M.&auinit=L.M.&auinit1=L&aulast=Bernardo
Citations (continued)
Cui, Jian, and Lawrence ISinoway. "Cardiovascular Responses to Heat Stress in Chronic Heart Failure." Current heart failure reports 11.2 (2014):139-145.
http://sfx.umd.edu/tu?sid=Elsevier%3AScopus&_service_type=getFullTxt&issn=15469530&isbn=&volume=11&issue=2&spage=139&epage=145&pages=139-145&artnum=&date=2014&id=doi%3A10.1007%2Fs11897-014-0191-y&title=Current%20Heart%20Failure%20Reports&atitle=Cardiovascular%20responses%20to%20heat%20stress%20in%20chronic%20heart%20failure&aufirst=J.&auinit=J.&auinit1=J&aulast=Cui